EVERYTHING YOU NEED TO KNOW ABOUT PILONIDAL CYSTS
Each year, around 70,000 Americans are diagnosed with pilonidal disease. Pilonidal disease is 2.2 times more common in males than females. Fortunately, the pilonidal cyst is a rare condition; therefore, it can easily be mixed up with other perianal diseases such as anal fistula and abscess of the perianal region. It is mainly treated surgically with a significant chance of recurrence, depending on the risk factors and lifestyle choices.
Table of Contents
WHAT IS PILONIDAL CYST?
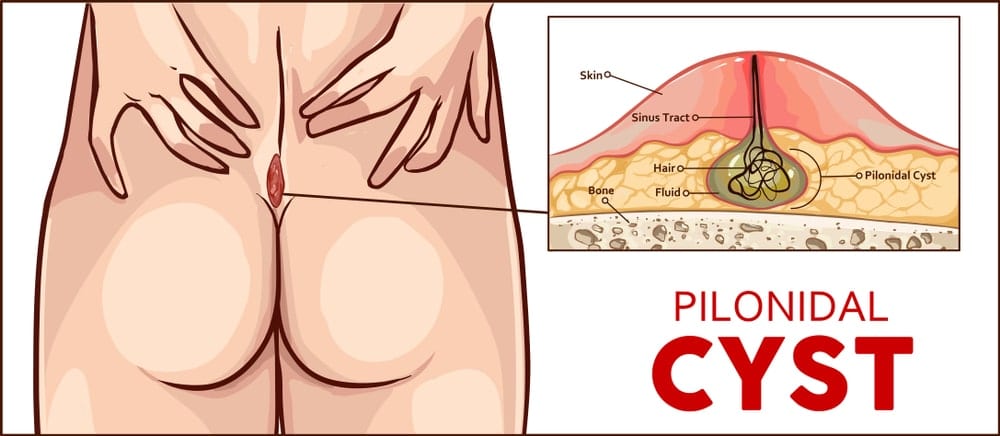
Pilonidal cysts are the fluid-filled sacs of tissue containing hairs and cellular debris that lies close to the crease of the buttocks and tailbone. Pilonidal cysts occur when coarse and small hairs penetrate the skin and become embedded into it. Later, they can form pus and cause a painful infection called “pilonidal abscess” or sinus cavities.
WHAT IS THE DIFFERENCE BETWEEN PILONIDAL CYST, PILONIDAL ABCESS, AND PILONIDAL SINUS?
A pilonidal cyst is simply a non-infectious fluid-filled cavity containing hairs mainly and other cellular debris and dirt. However, if the cyst is taken lightly, it can form a cavity and swelling of pus termed as a pilonidal abscess. After the infection, the pus will drain out through the pilonidal sinus (a small space formed in the skin and allows the drainage of the pus towards the outside).
WHAT ARE THE CAUSES OF PILONIDAL CYST?
A pilonidal cyst is mostly acquired due to the hairs being the main cause for the formation of a cyst. Conversely, it can be congenital due to the presence of post-coccygeal epithelium remnants since birth.
It is more prevalent among young males and males with a military background. The following are the causes of the pilonidal cyst that determine its susceptibility to disease.
- Young males (aged around 20s)
- Military background
- Prolonged sitting position
- Presence of a dimple on the skin around the tailbone
- Obesity
- Think hairy skin
- Tight clothing
- Any activity (such as cycling) that causes prolonged pressure on the crease of the bottom and forcing the penetration of hairs into the skin.
WHAT ARE THE RISK FACTORS OF PILONIDAL CYSTS?
The following are the risk factors for the occurrence of the pilonidal cysts.
- Male gender
- Young age around 20
- Diabetes
- Obesity
- Excess thick and coarse body hair
WHAT ARE THE COMMON SYMPTOMS OF PILONIDAL CYST?
Patients with pilonidal cyst don’t experience a wide variety of symptoms as the cysts are non-infectious. Localized symptoms around the tailbone are the main indications for the presence of cysts then generalized symptoms. If you have the pilonidal cysts, then you are likely to experience:
- Redness
- Swelling
- Pain
- Discharge of pus and sometimes blood
- Foul odor from the discharge
- Fever
Seek medical attention if you are experiencing any symptoms mentioned above.
HOW DO YOU DIAGNOSE PILONIDAL CYSTS?
Luckily, there’s no need for any pathological test or radiograph for the diagnosis of pilonidal cysts. A doctor will clinically examine the region around the tailbone to determine whether you have the pilonidal cysts. Ultrasound or MRI can be taken if the diagnosis is not clear.
WHAT ARE THE AVAILABLE TREATMENTS FOR PILONIDAL CYSTS?
There is no need to be afraid or stressed out if you have pilonidal cysts because of the availability of reliable treatments. Treatment can be divided into two broad categories – Non-operative treatment, operative treatment, or a combination of both treatments.
NON-OPERATIVE TREATMENT
It mostly depends on the efforts of patients, what a patient can do to reduce the occurrence and recurrence of pilonidal cysts. It mainly involves the lifestyle changes of patients.
- Weight loss and Exercise
- Maintenance of good and healthy hygiene
- Improve the way of habitual sittings
Hair removal treatment – Hairs being the main factor for the pathogenicity of the cysts, they can easily be removed by laser hair removal procedure or epilation such as waxing, shaving, or hair removal creams.It has been proved by many studies that laser hair removal treatment decreases the recurrence of pilonidal diseases. Usually, the recurrence rate of pilonidal disease is 13.3% with laser treatment. It is especially ideal for patients with sensitive skin and anal mucosal allergy to hair removal products.
OPERATIVE TREATMENT
Incision and drainage – Despite many non-operative available options, it is widely marked as a surgical procedure. The surgical treatment usually requires incision and drainage. The overall success rate of incision and drainage is 76%, and the overall recurrence rate of pilonidal disease is 21%. Initially, the local area is anesthetized for numbness. Once the area to be operated on is numb, a surgeon makes a small diamond-shaped cut in the lower back to drain out the hair follicles, fluid, and dirt. The wound will be left opened and packed with gauze.The healing period takes around 3 weeks, and regular dressing is needed until the wound is healed completely.
Advantages
- Removal of cysts
Disadvantages
- Painful dressing
- Doesn’t necessarily involve same-day discharge
- Bed rest needed
- Slow recovery of 3 weeks
Flap Surgery – Another treatment involves removing a flap of skin, but this procedure is avoided due to its complications. The downside of this treatment is the occurrence of flap necrosis in some patients.
Laser Surgery – Currently, the most advanced and less invasive treatment is laser treatment. A diode laser of 1470nm is used during the surgery.The laser treatment involves the excision of the pilonidal cyst area, and it can also treat the superior and inferior extensions. It involves a small 1cm cut instead of a flap or a larger cut.
Advantages
The advantages of laser surgery are
- Quick surgery
- Same-day discharge
- No bed rest needed
- No wound
- Painless dressing
WHAT IS THE POST-CARE OF PILONIDAL CYSTS’ TREATMENT?
The post-operative care for laser treatment involves:
- Take a painkiller if the pain is mild
- Antibiotics course of 3-4 days after the surgery
- Dressing
Conclusion
A pilonidal cyst can be a one-time problem or could be chronic (recurring). The pilonidal cyst doesn’t cause problems until they become infected; therefore, it shouldn’t be ignored or taken lightly. If you have a small or large pimple close to your tailbone, make sure to visit your doctor immediately for consultation and treatment. For more information, contact our Henderson clinic (702) 602-6600.
